Paid consultants help patients navigate Canada’s Byzantine health-care system
Andrée Colella had been in and out of hospital for months with bladder and bone infections when her husband, Tom, broke down and asked for help from an unconventional source: a private health-care advocate.
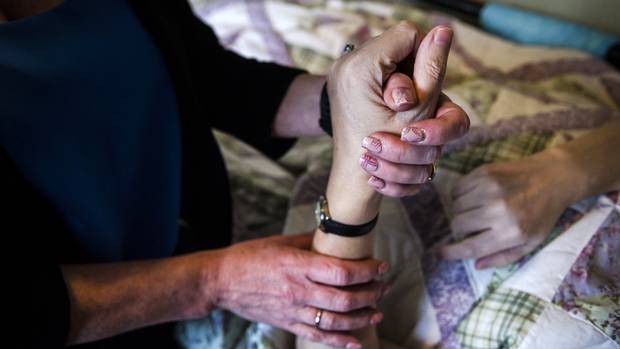
Patient navigator, Jana Bartley holds hands with her client Andree Colella, who suffers from multiple sclerosis, in Toronto on Tuesday, April 11, 2017. Christopher Katsarov for The Globe and Mail
Kelly Grant, The Globe and Mail April 14, 2017
For $90 an hour, Jana Bartley, a former obstetrics nurse and legal nurse consultant, took charge of the family’s case.
She organized meetings of the three agencies that care for Ms. Colella at home, where multiple sclerosis keeps the 60-year-old confined to a hospital bed in the kitchen. Ms. Bartley took minutes at the gatherings and set goals for Ms. Colella’s care, including reducing the number of nurses and personal-support workers who cycled through the couple’s modest house in east Toronto.
With consistent care from a few providers who know Ms. Colella well, her health has improved.
“I could not have solved my current situation if I didn’t have Jana to support me at a time when I needed it,” said Mr. Colella, 69, a retired engineering assistant who works part-time as an educational assistant for students with special needs.
Ms. Bartley, founder of Toronto-based Integrity Healthcare Consultants, is part of a small but growing new field of private advocates or navigators who will – for a fee – help patients and their families find their way through Canada’s labyrinthine health-care system. (Navigators and case managers exist within the public system, too, typically in cancer care. But they are employed and paid for by hospitals or health authorities, not by patients).
Private patient navigators review medical files, attend doctors’ appointments, book tests, chase down specialists and co-ordinate in-home care, often for elderly clients with chronic illnesses whose grown children live far away. For those who can afford to pay, the service can be a godsend.
But the advent of a private patient advocacy profession in Canada also raises questions about how impenetrable the public health-care system has become, and how appropriate it is for those with the means to buy their own squeaky wheel.
“I can understand people feeling overwhelmed or not understanding the system or wanting someone to help co-ordinate care,” said Monika Dutt, a Nova Scotia family physician and the chair of Canadian Doctors for Medicare. “But it does create inequity in who can access what care.”

It’s hunting season every season in Canada if you are a taxpayer. Monitor Telegram
Private patient advocacy is more common in the United States than in Canada, according to Trisha Torrey, executive director of the Alliance of Professional Health Advocates, which represents independent health advocates and case managers.
The alliance has about 630 members, approximately two dozen of whom are Canadian, she said. Most have a medical background, but some are former patients or relatives of patients who are now using their knowledge of the health-care system to make a living. Anyone can hang out a shingle as a patient advocate.
That is about to change, Ms. Torrey said. She sits on the Patient Advocate Certification Board, which has spent four years developing a certification test and credentialing system for patient advocates that will be open to Canadians. She predicts the first group will be certified by the second quarter of next year.
In the meantime, a handful of patient advocacy companies have opened in Canada in the past couple of years, including operations in Toronto, Ottawa, Saskatoon and Victoria.
Susan Hagar founded Ottawa-based Nurse On Board in early 2015. Just last month, she expanded to Oakville, Ont., west of Toronto. She is one of seven nurses employed by the company, which charges $250 for an initial intake appointment and between $100 and $125 an hour, depending on whether clients pay a retainer fee.
“What is very common,” she said, “is that adult children are reaching out to us. Often the sandwich generation is really suffering with the caregiving role.”
That was the case for Ethan Armit, a 34-year-old Sudbury mining technician whose father, Allan, who ended up in hospital in three different facilities over 11 months after a heart attack in February, 2016.
The elder Mr. Armit, now 68, had a history of mental illness and lived a six-hour-drive away, in Kingston, at the time. That made care co-ordination a challenge for Ethan, who has a young family of his own.
After finding Nurse on Board through a Google search, the younger Mr. Armit met with Ms. Hagar and started paying for regular help from another nurse, Lynn Joseph.
She drove to Kingston every week to check on Mr. Armit’s father, instructed the hospital to taper his medications, helped compose a legal letter when a hospital wouldn’t stop heavily sedating him, and translated medical jargon into lay language for him.
All told, the service cost an average of $1,500 a month, money that came out of the elder Mr. Armit’s teacher’s pension.
“I would have paid 10 times that for what they’ve done,” the younger Mr. Armit said. “They’ve probably saved my marriage and they provided me with the ability to spend time with my son.”
Some of the doctors and nurses Mr. Armit encountered embraced Ms. Joseph’s help. Others got their backs up.
“It was always a point of controversy when we’d show up at one of these new hospitals with our patient advocate,” he said. “They just didn’t know why she was here. [They would ask,] ‘Is she here to watch us? Is she here to question us?’”
Ms. Hagar said that although she and her colleagues are usually received warmly by doctors, she is wary of setting up an adversarial situation. Her company has dropped the title advocates in favour of “care managers.”
Paul Hacker, a palliative-care physician in Ottawa who treats patients in their homes, said he would welcome the opportunity to work with private navigators or case managers. They could lift some of the organizational burden from doctors and family caregivers.
“It’s a huge stress on the non-patient. They don’t know what they’re supposed to do. So if there was a navigator working with me on patients like that, I’d be happy,” he said. “But those are sometimes the people who can least afford a private option.”
 Source The Globe and Mail
Source The Globe and Mail
Patient navigators becoming the norm in Canada, Erin Walkinshaw. CMAJ. October 18, 2011 vol. 183 no. 15 First published September 19, 2011, doi: 10.1503/cmaj.109-3974
Also see
What Should Primary Care Look Like in the Future? in The Medical Futurist
Should the wealthy be allowed to buy their way to faster health care at private clinics? in The Toronto Star
Your Little Ol’ Canadian Goose Is Being Cooked in The Monitor Telegram
